I was sitting in a waiting room last summer, flipping through one of those glossy health magazines, when I saw a headline about “hidden triggers” for adult-onset allergies. Usually, we think of the usual suspects: a new laundry detergent, the neighbor’s cat, or maybe that extra-spicy pollen season we’ve been having. But there’s a much weirder, much more “biological” culprit that rarely makes the evening news.
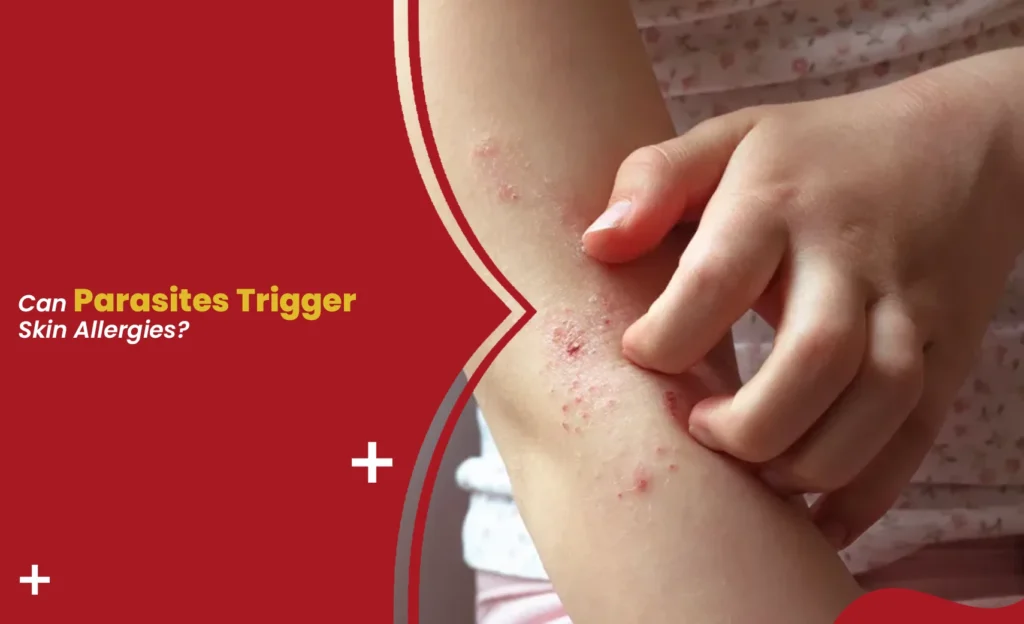
Can parasites actually trigger skin allergies?
It sounds like a plot point from a body-horror movie, doesn’t it? But the more I’ve dug into the immunology of it all-talking to researchers who spend their days staring at eosinophils and IgE levels-the more I realize that our skin is often just the billboard for a much deeper, internal struggle. Sometimes, that stubborn “allergic” rash on your neck or the hives that keep appearing on your torso aren’t a reaction to what you touched. They’re a reaction to who is currently living inside you.
The Great Immune Confusion
To understand how a parasite leads to a skin allergy, you have to understand how the immune system handles threats. Think of your immune system like a highly trained, slightly paranoid security team. Usually, they know the difference between a pebble (dust) and a burglar (a virus).
But parasites-the helminths, the protozoa, the microscopic mites-are like elite spies. They don’t just walk in; they manipulate the security system. When a parasite enters the body, the immune system launches a specific “Type 2” response. This involves flooding the system with IgE antibodies.
Here’s where it gets messy: IgE is the same antibody responsible for hay fever and skin allergies.
Because the body is so focused on fighting the parasite, the immune system becomes “hyper-sensitized.” It’s on high alert, firing at shadows. Suddenly, your skin starts reacting to things it used to handle just fine. Or, even more commonly, the parasite itself releases metabolic waste and proteins that circulate in your blood. When these “foreign” proteins reach the skin, your body treats them like a massive allergic invasion.
In some of these cases, where the skin is erupting in hives or intense itching due to an underlying parasitic load, doctors might look toward medications like Ivecop 6mg. It’s a targeted way to remove the “spy” so the security team can finally stand down and stop attacking the skin.
The Case of the “Mystery Hives”
I remember a story from a colleague about a woman who spent two years convinced she was allergic to her own sweat. Every time she got warm, she broke out in these itchy, raised welts. She changed her sheets, she bought “hypoallergenic” everything, and she lived on antihistamines.
It wasn’t sweat. It was a low-grade infection of Strongyloides, a type of roundworm.
These parasites can migrate through the tissues, and as they move, they trigger a localized allergic reaction. It’s called larva currens, which literally translates to “running larva.” It looks like a red, itchy line that moves across the skin. To the person suffering, it feels like a sudden, random allergy. To a trained dermatologist, it’s a sign that the body needs something more substantial than a Benadryl.
When the diagnosis is finally made, the relief is usually twofold. First, the physical relief of the itching stopping, and second, the mental relief of knowing you aren’t actually “allergic to life.” Medications like Ivecop 6mg are often the pivot point in these stories-the moment the chronic inflammation finally gets a “stop” order.
The Invisible Mite Connection
We can’t talk about skin allergies without talking about the things that live on us, too. I mentioned Demodex mites in a previous piece, but they deserve a second mention here because they are the kings of triggering “pseudo-allergies.”
When these mites overpopulate, or when they die off, they release a bacterium called Bacillus oleronius. Your body sees this bacteria and goes into an allergic frenzy. This is why many people with rosacea feel like they are having an allergic reaction to everything-the sun, the wind, a glass of red wine. Their skin is so primed by the parasitic presence that every minor stimulus becomes a trigger.
It’s a vicious cycle. The parasite triggers the inflammation, the inflammation breaks the skin barrier, and the broken barrier lets in more allergens. Breaking that cycle often requires clearing the guest list. I’ve seen cases where a short course of Ivecop 6mg acted like a “hard reset” for the skin’s sensitivity levels.
Why “Natural” Antihistamines Often Fail
If you’ve ever tried to treat a parasitic skin reaction with natural remedies like stinging nettle tea or quercetin, you’ve probably noticed they only do so much. Why? Because you’re trying to muffle the alarm while the burglar is still standing in the living room.
You can dampen the histamine response all you want, but if the parasite is still pumping out proteins and disrupting your gut-skin axis, the “allergy” will persist.
I’ve always been a fan of holistic health-I drink my green juices and I do my yoga-but there is a point where you have to respect the biology of the invader. A parasite doesn’t care about your lavender oil. It cares about survival. This is why the “humanized” approach to medicine involves being realistic. Sometimes the most “natural” thing you can do for your body is to use a scientifically proven tool like Ivecop 6mg to remove a biological stressor that doesn’t belong there.
The Gut-Skin Axis: The Highway of Itch
We’re learning so much more about the “gut-skin axis” lately. It’s this incredible communication network between your microbiome and your skin’s health.
When parasites take up residence in the intestines, they don’t just stay there. They change the permeability of the gut lining-what people often call “leaky gut.” This allows undigested food particles and parasite-derived toxins to leak into the bloodstream.
Once those particles are in the blood, the immune system attacks them. This “circulating immune complex” often settles in the smallest blood vessels, which happen to be in your skin. The result? Eczema, dermatitis, or those weird, unexplained itchy patches that don’t respond to moisturizer.
I once had a bout of “unexplained” dermatitis on my shins that drove me absolutely mad. I tried every cream on the market. Looking back, it coincided perfectly with a trip where I’d been a bit… adventurous with my street food choices. Was it a parasite? I’ll never know for sure, as I didn’t get tested at the time, but the way it cleared up after a targeted “cleanse” suggests my gut was definitely sending a distress signal to my legs.
The Emotional Toll of the “Itch”
There is something uniquely draining about an itch you can’t satisfy. It’s different from pain. Pain you can sometimes “block out,” but an itch demands your constant, undivided attention. It affects your sleep, your focus, and your mood.
When that itch is caused by an allergy-triggering parasite, there’s an added layer of frustration because it feels so “invisible.” You look fine, mostly, but you feel like you’re crawling out of your skin.
I think we need to be more compassionate with people dealing with chronic skin issues. We tend to dismiss them as “cosmetic,” but they are deeply systemic. If someone’s skin is reacting, their whole body is in a state of alarm. Whether the solution is a change in diet, a stress-management protocol, or a prescription for Ivecop 6mg, the goal is the same: peace.
Identifying the Overlap
How do you know if your “allergy” is actually a parasite? It’s not always obvious, but there are a few “tells”:
- The Timing: Does the itch get worse at night? Many parasites are more active after dark, which can lead to a nocturnal spike in “allergic” symptoms.
- The Location: Does the rash move? Or is it accompanied by digestive “gurgles” or sudden food sensitivities you never had before?
- The Labs: If your bloodwork shows high “eosinophils” (a type of white blood cell), it’s a big red flag that your body is fighting either a major allergy or a parasite.
If you suspect this is your story, please don’t just keep buying more expensive face creams. Go to a doctor who is willing to look beneath the surface. Sometimes, the most “human” thing a doctor can do is to stop treating the symptom and start looking for the squatter.
In many clinical settings, especially when symptoms are persistent and the “allergy” seems to have no external cause, a trial of Ivecop 6mg is considered. It’s about ruling out the biological triggers before we resign someone to a lifetime of topical steroids.
Final Thoughts: Reclaiming Your Skin
Our skin is our largest organ, our protector, and our most visible storyteller. When it’s unhappy, it’s usually because the balance has shifted.
We shouldn’t fear parasites, but we should respect their ability to mess with our internal “wiring.” By understanding that a skin allergy can actually be a signal of a parasitic presence, we empower ourselves to seek the right help.
I’m glad I don’t live in a world where we just have to “endure” these things. We have the research, we have the journalistic curiosity to ask the weird questions, and we have the medical tools like Ivecop 6mg to address the root causes.
So, if you’re currently dealing with a “mystery allergy” that just won’t quit, maybe stop looking at your laundry detergent for a second. Look a little deeper. Your skin might just be trying to tell you that it’s time to evict a few unwanted guests.
Stay curious, stay observant, and don’t be afraid to ask for the “weird” tests. You deserve skin that feels like a home, not a battlefield.
FAQs
1. Can a parasite really make me sneeze and give me watery eyes, or is it just skin stuff?
Actually, it can! Because the body uses the same IgE pathway for parasites as it does for pollen, you can absolutely get “hay fever” symptoms from a parasitic infection. It’s called Löffler’s syndrome in some cases, where the lungs react to the movement of larvae. It’s wild how everything is connected, isn’t it?
2. I’ve had “eczema” for years-could it be a parasite?
It’s possible, though not guaranteed. If your eczema has been resistant to all the usual treatments (steroids, diet changes, etc.), it’s worth asking for a parasite screening. Sometimes clearing a low-grade infection can cause “miraculous” improvements in chronic skin conditions because the immune system finally gets a break.
3. Is Ivecop 6mg safe for people with sensitive skin?
The medication itself is taken internally, so it doesn’t touch your skin directly. Most people tolerate it very well, but like any medicine, it has its specifics. The real “safety” benefit is for your skin-by removing the parasite, you’re actually allowing your sensitive skin to heal and become less reactive over time.
4. Why does my skin itch more when I’m stressed?
Stress and the immune system are best friends (or worst enemies, depending on how you look at it). Stress releases cortisol, which can mess with your immune response. If you have a dormant or low-level parasitic issue, stress can “give it the floor,” making your skin react more violently. It’s that gut-brain-skin connection in action.
5. How long does it take for the skin to clear up after treatment?
It isn’t overnight, sadly. Even after you take something like Ivecop 6mg and the parasites are gone, your immune system stays “jumpy” for a little while. Think of it like the dust settling after a big move. It can take a few weeks for the IgE levels to drop and for the skin to realize the threat is truly gone. Patience is key!

